Dental Insurance Terms Explained for Families
Dental Insurance Terms Explained for Families

Trying to figure out dental insurance often feels confusing when words like deductible, copay, and coinsurance appear in every conversation. For Spanish-speaking families in San Bernardino, every dollar counts, and misunderstanding these insurance terms can mean extra stress or missed benefits. Learning the meaning behind important phrases like “annual maximum” and “assignment of benefits” puts you in the driver’s seat, helping your family get the most from your Denti-Cal plan and avoid unplanned expenses. Let’s simplify these dental insurance basics so you can feel confident every time you visit your dentist.
Table of Contents
- Dental Insurance Terms All Patients Should Know
- Comparing Denti-Cal, PPO, and HMO Plans
- Key Features of Dental Coverage Options
- Common Costs: Premiums, Copays, and Deductibles
- Maximizing Your Dental Benefits Safely
Key Takeaways
| Point | Details |
|---|---|
| Understand Key Terms | Familiarize yourself with essential dental insurance terms like deductible, copay, and coinsurance to manage costs effectively. |
| Choose the Right Plan | Select a dental insurance plan (Denti-Cal, PPO, or HMO) based on your financial situation and dentist preferences for optimal care. |
| Maximize Preventive Care | Schedule preventive visits early in the year to fully utilize your benefits and catch issues before they require more expensive treatment. |
| Plan for Major Services | Strategically time major dental work around your annual maximum and deductible resets to optimize coverage use and manage out-of-pocket costs. |
Dental Insurance Terms All Patients Should Know
When you’re shopping for dental insurance or trying to understand a benefits statement, the language can feel like reading a foreign textbook. Terms like deductible, copay, and coinsurance get thrown around without explanation, leaving families confused about what they’ll actually pay out of pocket. For Spanish-speaking families in San Bernardino managing tight budgets, understanding these key terms isn’t just helpful—it’s essential for maximizing your benefits and avoiding surprise bills. Knowing what common dental insurance terms mean puts you in control of your dental spending and helps you make informed decisions about which plan works best for your family.
Let’s break down the terms you’ll encounter most often:
-
Deductible: This is the amount you pay out of your own pocket before your insurance kicks in. If your plan has a $100 deductible and you need a filling, you pay $100 first, then insurance covers the rest (based on your plan). Many Denti-Cal plans in California have low or no deductibles, which is one reason families find them affordable.
-
Copay: A fixed amount you pay for each visit or service. You might pay $0 for a regular checkup and $25 for a filling. It’s straightforward and predictable.
-
Coinsurance: After you meet your deductible, coinsurance is the percentage of costs you split with insurance. If coinsurance is 20 percent, you pay 20 percent and insurance covers 80 percent. This applies to many procedures like root canals or crowns.
-
Allowed charge (also called allowed amount): This is the maximum amount your insurance company will consider for payment. Even if your dentist charges more, the insurance calculation starts here. At Monteluz Dental, we accept assignment of benefits, meaning we bill insurance directly and you’re only responsible for your portion.
-
Assignment of benefits: When you authorize your dentist to bill insurance directly and receive payment instead of you getting reimbursed. This reduces your paperwork and often means you pay less upfront.
-
Benefit limits and annual maximums: Most plans cap how much they’ll pay per year (typically $1,000 to $2,000). Once you hit that limit, you pay 100 percent for remaining care that year. Plan ahead to make the most of your benefits.
-
Waiting periods: Some plans have waiting periods before covering specific procedures like crowns or implants. Denti-Cal and many employer plans have different waiting periods, so check your specific plan details.
Understanding these dental insurance terms and coverage policies helps you predict costs and avoid bill shock. When you know the difference between a copay and coinsurance, you can budget better. When you understand your annual maximum, you can prioritize needed procedures strategically. For families using Denti-Cal benefits, many preventive services like cleanings, exams, and X-rays are covered at 100 percent, which means you focus your annual maximum on more complex procedures like root canals or extractions.
Here’s a quick reference guide to help you understand essential dental insurance terms and their impact on your budget:
| Term | What It Means | How It Impacts Costs |
|---|---|---|
| Deductible | Amount paid before coverage begins | Sets initial out-of-pocket |
| Copay | Fixed fee per service or visit | Predictable visit expenses |
| Coinsurance | Percentage split after deductible | Affects cost-sharing ratio |
| Allowed Charge | Max cost insurance will consider | Limits insurer payouts |
| Assignment of Benefits | Dentist bills insurance directly | Less paperwork for patients |
| Annual Maximum | Yearly coverage cap by insurer | Out-of-pocket after max |
| Waiting Period | Time before coverage starts for services | Delays access to procedures |
The best approach is to call your dentist’s office (or call us at Monteluz Dental) with your insurance information and ask for a cost estimate before treatment. We can tell you exactly what your insurance will cover, what your copay or coinsurance is, and whether the procedure counts toward your annual maximum. This conversation takes 10 minutes and saves you from unexpected costs later.
Pro tip: Keep a copy of your insurance card and plan summary in your phone or wallet, and don’t hesitate to ask your dentist’s office to explain the breakdown of costs before any procedure—most dental offices, including ours, are happy to walk you through the numbers so there are no surprises.
Comparing Denti-Cal, PPO, and HMO Plans
Choosing a dental insurance plan feels overwhelming when you’re juggling family budgets and trying to understand what each option actually covers. For Spanish-speaking families in San Bernardino, the choice often comes down to three main plans: Denti-Cal (California’s public dental program), PPO plans, or HMO plans. Each works differently, costs differently, and gives you different choices about which dentist you see. Understanding how these common dental plan types differ helps you pick the one that matches your family’s needs and budget.
How Each Plan Works
Denti-Cal is California’s Medicaid dental program designed for low-income individuals and families. If you qualify based on income, Denti-Cal covers a broad range of services including cleanings, fillings, root canals, extractions, and dentures. You go to any dentist who accepts Denti-Cal (including Monteluz Dental), and there’s usually no copay or deductible. The tradeoff is that not every dentist accepts Denti-Cal, and you might wait longer for appointments since it’s a public program with high demand.
PPO plans (Preferred Provider Organizations) give you the most flexibility. You can see any dentist you want, whether they’re in-network or not. In-network dentists are cheaper because your insurance has negotiated rates with them. If you go out-of-network, you pay more (higher coinsurance), but you still get some insurance coverage. PPO plans usually have higher monthly premiums ($30-$60 or more), a deductible ($50-$200), and coinsurance that splits costs with you. You have freedom to choose your dentist, which appeals to families with established relationships with specific providers.
HMO plans (Health Maintenance Organizations) work the opposite way. You choose one primary care dentist from an approved network, and you go to that dentist for most care. If you need a specialist, your primary dentist refers you to someone in-network. HMOs have lower premiums (sometimes under $20 monthly) and fixed copays ($0-$25 per visit), making them predictable and budget-friendly. The tradeoff is restricted choice. Go out-of-network without approval, and you pay the full bill yourself.
Here’s a side-by-side comparison:
| Feature | Denti-Cal | PPO | HMO |
|---|---|---|---|
| Cost per month | Free or low-cost | $30-$60+ | Under $20 typically |
| Copay/Deductible | Usually none | $50-$200 deductible, copay $0-$50 | $0-$25 fixed copay |
| Dentist choice | Any Denti-Cal provider | Any dentist (higher cost out-of-network) | One primary dentist in-network |
| Coverage | Comprehensive for eligible patients | Preventive 100%, major 50-80% | Preventive 100%, major 50-80% |
| Best for | Low-income families | Families who value choice | Families wanting predictable costs |
Which Plan Fits Your Family?
If your family income qualifies, Denti-Cal is hard to beat. You get comprehensive coverage with minimal costs. At Monteluz Dental, we accept Denti-Cal and understand how to maximize your benefits. Apply through the California Department of Health Care Services website to check eligibility.
If your family earns above Denti-Cal limits but wants flexibility, a PPO plan works well if you can handle higher monthly costs. You pay more upfront but get dentist choice.
If you want the lowest monthly payment and have a trusted dentist you like, an HMO plan locks in predictable costs. Just make sure your preferred dentist is in-network before signing up. Many dental offices, including Monteluz Dental, participate in multiple insurance networks, so check our accepted plans when you call.
Understanding dental coverage options helps you match your family’s dental needs with a plan you can actually afford. Don’t just pick the cheapest plan. Pick the one that covers the procedures your family needs at costs you can handle.
Pro tip: Before enrolling in any plan, call the dentist’s office you want to use and confirm they accept that insurance plan and whether you need a referral for specialists—this 5-minute call saves you from discovering plan incompatibility after enrollment.
Key Features of Dental Coverage Options
Dental plans look similar on the surface, but the details buried in the fine print make huge differences in what you actually pay and what you can access. When you’re comparing plans for your family, you need to understand the specific features that determine your real out-of-pocket costs and coverage limits. For Spanish-speaking families in San Bernardino managing tight budgets, knowing these features means the difference between affording the dental care your family needs and putting it off because bills feel overwhelming.

Understanding Coverage Tiers
Most dental plans divide services into three categories, and each tier has different coverage percentages. Learning about dental plan design and coverage percentages helps you predict exactly what you’ll pay for different procedures.
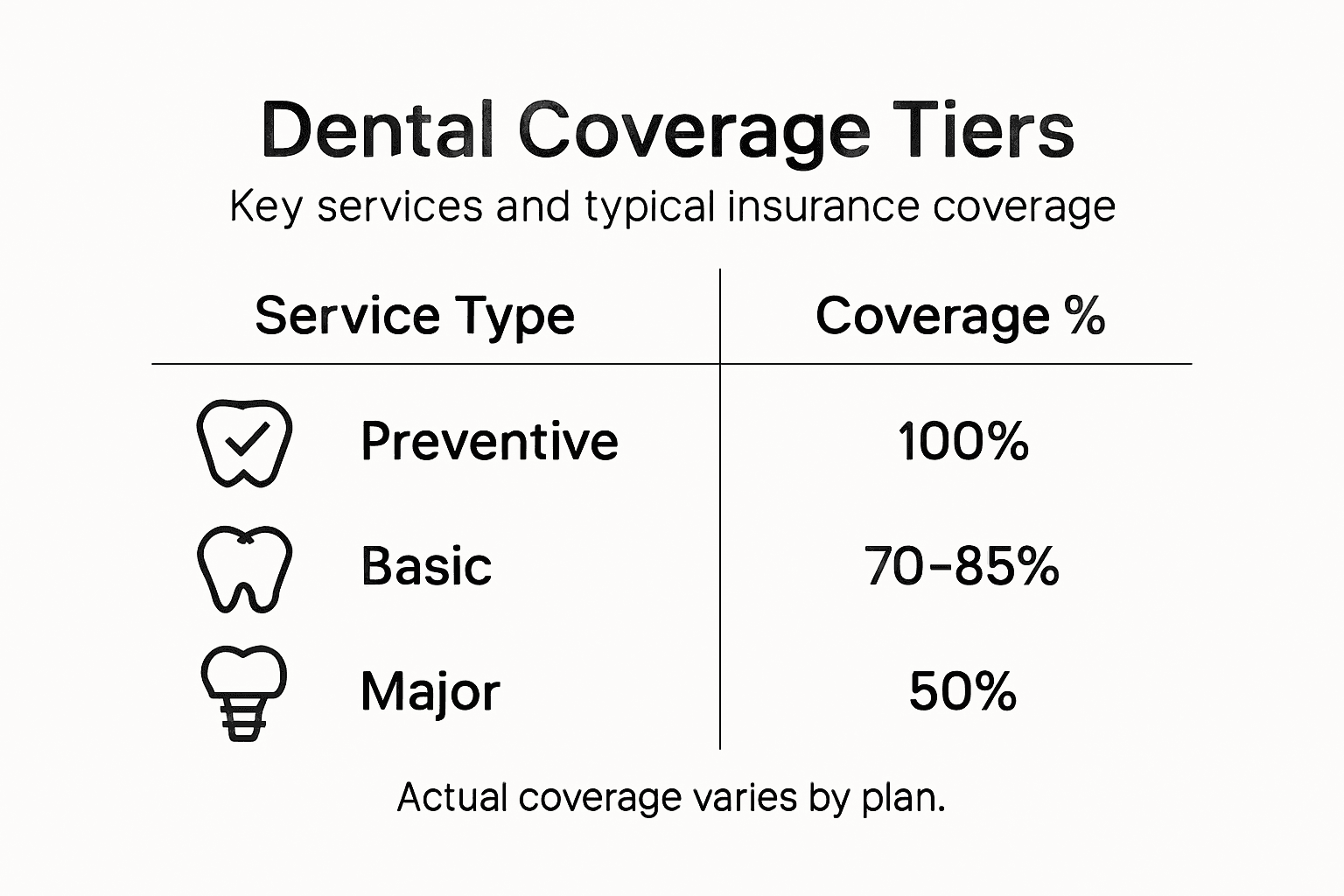
Preventive services (cleanings, exams, X-rays, fluoride) are typically covered at 100 percent with no copay. This is true across almost all plans because insurers know prevention saves money long-term. You can go twice yearly for cleanings at no cost.
Basic services (fillings, extractions, simple root canals) are usually covered at 70-85 percent. This means you pay 15-30 percent and insurance pays the rest. A filling that costs $200 might mean you pay $30-$60 out of pocket.
Major services (crowns, bridges, implants, complex root canals) are typically covered at 50 percent. You pay half, insurance pays half. A crown costing $1,200 means you pay around $600. This is why understanding annual maximums (covered below) matters so much.
To see how dental coverage tiers affect costs, here’s a simple breakdown for typical procedures:
| Service Type | Typical Coverage % | Example Cost to Patient (if procedure is $200) |
|---|---|---|
| Preventive (cleaning, exam) | 100% | $0 |
| Basic (filling, extraction) | 70-85% | $30–$60 |
| Major (crown, implant) | 50% | $100 |
| Orthodontics | Up to 50% | Varies, often strict limits |
Some plans also cover orthodontics at 50 percent, but coverage limits are strict.
The Annual Maximum and Waiting Periods
Here’s the reality that surprises most families: your insurance doesn’t cover unlimited care. Most plans cap benefits at $1,000 to $2,000 annually. Once you hit that cap, you pay 100 percent for any remaining services that year. If your family has multiple people needing expensive work (crowns, extractions, root canals), you might blow through your annual maximum by October.
Waiting periods are another feature that affects your actual coverage. Many PPO and HMO plans have waiting periods ranging from 6 months to a year before they cover basic and major services. Denti-Cal typically has no waiting period. This means if you enroll in a new PPO plan in January needing a crown, you might have to wait until July before insurance covers it.
Some plans waive waiting periods if you had continuous coverage with another plan, so ask about this when enrolling.
Network Restrictions and Negotiated Fees
Your plan’s network affects what you actually pay. In-network dentists have agreements with your insurance company and accept negotiated lower fees. Out-of-network dentists charge their own fees, which are often much higher. Your insurance calculates benefits based on the negotiated in-network fee, not the dentist’s actual charge. So going out-of-network costs more in two ways: higher actual fees plus higher coinsurance percentages.
At Monteluz Dental, we participate in multiple networks including Denti-Cal, PPO, and HMO plans. We understand dental insurance benefit structures and help families maximize their coverage. When you call with your insurance card, we can tell you exactly what your negotiated fees are and what you’ll pay for each procedure.
Putting It All Together
Let’s say your family has a PPO plan with a $100 deductible, 80 percent coverage for basic services, 50 percent for major, and a $1,500 annual maximum. Your child needs two fillings ($200 each) and a crown ($1,200). Here’s your actual cost:
- Pay the $100 deductible first
- Two fillings at $400 total: Insurance covers 80 percent ($320), you pay 20 percent ($80)
- Crown at $1,200: Insurance covers 50 percent ($600), you pay 50 percent ($600)
- Your total out-of-pocket: $100 + $80 + $600 = $780
- Insurance paid: $920
- Remaining annual maximum: $580 (you have $1,500 - $920 = $580 left for the rest of the year)
This breakdown shows why understanding features matters. You need to know your deductible, coverage percentages, and annual maximum to budget for dental care realistically.
Pro tip: Request an itemized cost estimate from your dentist’s office before any major procedure, showing the procedure cost, what insurance will cover, and exactly what you’ll pay out-of-pocket—this eliminates surprises and lets you plan financially.
Common Costs: Premiums, Copays, and Deductibles
Dental insurance costs come in multiple pieces, and unless you understand each one, your family budget can get blindsided. You might think a low premium means cheap insurance, then discover you owe $500 per visit in copays. Or you might assume deductibles only apply once per year, then find out they reset for each family member. For Spanish-speaking families in San Bernardino, understanding these three cost categories means you can actually predict what you’ll pay and choose a plan that fits your budget without surprises.
Premiums: Your Monthly Insurance Payment
A premium is what you pay monthly to keep your insurance active. This amount stays the same every month regardless of whether you go to the dentist or not. Premiums vary widely based on plan type and coverage level.
Denti-Cal has minimal or no premium for qualifying families. PPO plans typically range from $30 to $60 monthly per person, sometimes higher depending on coverage. HMO plans usually cost $10 to $25 monthly, occasionally less. Some employer plans have higher premiums but better coverage. The key: a low premium doesn’t mean good value if you end up paying thousands in copays and deductibles.
Think of your premium like a monthly subscription. You pay it whether you use your benefits that month or not. For families who see the dentist regularly, a higher premium with better coverage might cost less overall than a cheap premium with high copays.
Copays: The Fixed Fee Per Visit
A copay is a fixed amount you pay when you receive a service. Understanding dental insurance cost structures and copayments helps you budget for regular visits.
Here’s how copays typically work:
- Preventive visits (cleaning, exam, X-rays): $0 to $25 copay
- Fillings or extractions: $25 to $50 copay
- Root canals or crowns: $50 to $100 copay
- Specialist visits (orthodontist, periodontist): $50 to $100 copay
The beauty of copays is predictability. You know exactly what you’ll pay. Many Denti-Cal plans have zero copay for preventive care and low copays for other services, making them budget-friendly for families. HMO plans typically have fixed copays too, which is why families like them. PPO plans sometimes use copays for preventive care but coinsurance (a percentage) for everything else.
Deductibles: What You Pay Before Insurance Helps
A deductible is the amount you pay out of pocket before your insurance starts covering costs. Once you’ve paid your deductible for the year, your copay or coinsurance kicks in. Family deductibles can apply per person or to the entire household.
Typical deductibles range from $0 to $200 annually. Denti-Cal usually has no deductible. Some PPO plans have $50 deductibles, others $150 or $200. HMO plans often have zero deductibles. Here’s the catch: the deductible typically applies only to basic and major services, not preventive care. This means you can go to your cleaning at no cost even if you haven’t met your deductible.
Families with multiple people need to understand whether the deductible is individual or family. If you have a $100 individual deductible, each family member pays $100 before coverage kicks in. If it’s a $300 family deductible, only $300 total is due from your entire household before insurance covers everyone.
Real Example: Putting It Together
Let’s say your family chose an HMO plan: $20 monthly premium, $0 deductible, $25 copay per visit. Your child gets a cavity and needs a filling.
- Monthly premium you’ve already paid: $20 (counts toward insurance, you don’t pay extra)
- Copay at the visit: $25
- Your total cost for that filling: $25
Compare this to a PPO plan: $50 monthly premium, $100 deductible, $25 copay per preventive visit, $50 copay for filling, and 20 percent coinsurance for major work.
- Monthly premium: $50 (already paid)
- Deductible toward filling: $100
- Copay at visit: $50
- Filling costs $200, you pay 20 percent coinsurance: $40
- Your total cost for that filling: $100 + $50 + $40 = $190
The PPO looks expensive upfront, but it gives you dentist choice. The HMO costs less out-of-pocket but locks you into one dentist.
Understanding dental plan cost components and explanation of benefits helps you review your insurance card and explanation of benefits (EOB) statements. These documents show you exactly what your plan charges and what you’ll owe.
Pro tip: Write down your premium amount, deductible, copay amounts for different service types, and annual maximum on a note in your phone so you have this information instantly when calling your dentist for cost estimates.
Maximizing Your Dental Benefits Safely
Having dental insurance is only half the battle. The real advantage comes from using your benefits strategically so you get the care your family needs without wasting coverage or creating financial stress. For Spanish-speaking families in San Bernardino managing limited budgets, maximizing benefits means planning ahead, understanding what your plan covers, and making smart choices about when and where you seek care. The goal is to use your full annual benefit without overspending, while maintaining good oral health throughout the year.
Start with Prevention
Prevention is the single best way to maximize benefits safely. Nearly every plan covers preventive services (cleanings, exams, X-rays, fluoride) at 100 percent with no copay. These visits cost you nothing and save your insurance company thousands by catching problems early. If you skip preventive care to save money, you end up needing expensive treatments later that count against your annual maximum.
Schedule your family’s preventive visits at the beginning of the year, ideally January or February. This gives you the full year to use your remaining benefits for needed treatments. Children should visit twice yearly, adults at least once. If your family hasn’t had checkups in years, catch up now. Many plans waive waiting periods for preventive care, so even new insurance can cover your first cleaning immediately.
Think of preventive care as free money from your insurance company. Using those benefits protects your actual budget for other expenses.
Understand Your Plan Before You Need Care
Before you have a dental emergency or need expensive work, read your insurance documents completely. Call your insurance company or dentist’s office with these questions:
- What is my annual maximum benefit amount?
- Does my plan have a waiting period for basic or major services?
- Which dentists are in-network?
- What is my deductible and does it apply to preventive care?
- What percentage does insurance cover for basic services? Major services?
- Are there any exclusions or services not covered?
Writing down these answers prevents surprises. When you know your annual maximum is $1,500 and you’re in September, you can plan whether to schedule that crown before year-end or wait until January when your benefits reset.
Understanding how to optimize dental benefits safely through preventive care and smart plan use ensures your family gets maximum value from coverage.
Choose In-Network Providers
In-network dentists have negotiated rates with your insurance, which means lower fees and better coverage percentages. Going out-of-network costs significantly more. Your insurance calculates benefits on the out-of-network’s higher fee, and you pay a larger percentage coinsurance. The difference can easily be $200 to $500 per procedure.
At Monteluz Dental, we participate in multiple insurance networks including Denti-Cal, PPO, and HMO plans. We understand how to maximize your benefits and bill insurance correctly so you pay less. When you call, tell us your insurance plan and we can confirm you’re in-network and provide exact cost estimates.
Plan Major Work Strategically
If your family needs expensive procedures (crowns, root canals, implants, extractions), plan the timing around your annual maximum and deductible reset. If you’re mid-year and still have $1,200 in benefits available, schedule that crown now. If you’re in November with only $300 left, consider waiting until January when benefits reset unless the procedure is urgent.
For families with multiple people needing work, stagger procedures if possible. Have one person get their crown in December while another person gets fillings in January to spread the annual maximum use across two benefit years.
Get cost estimates in writing before agreeing to treatment. Ask your dentist to show you what insurance will cover and what you’ll owe. This planning prevents bill shock and lets you budget for dental expenses like any other household cost.
Maintain Continuity Throughout the Year
Don’t abandon dental care mid-year because you hit your deductible or ran out of insurance coverage. Many families stop going after their annual maximum is exhausted, then return in January with new problems. This costs more in the long run. Preventive care during months when insurance won’t pay is still cheaper than treating problems that develop from neglect.
If you need care after your annual maximum is used, ask your dentist about payment plans or discounts. Many offices, including Monteluz Dental, offer in-house payment plans or membership programs (ours starts at just $20 monthly) to help uninsured or post-maximum patients.
Pro tip: Schedule your preventive visit in January, ask your dentist to identify any needed treatments and their costs, then create a written plan for the year showing which procedures fit within your annual maximum and which to schedule when benefits reset.
Understand Your Dental Insurance and Take Control of Your Family’s Care Today
Navigating dental insurance terms like deductible, copay, and coinsurance can feel overwhelming but knowing them empowers your family to make informed decisions and avoid unexpected costs. If you want to stop worrying about confusing coverage details and start maximizing your benefits effectively, Monteluz Dental Specialty Group in San Bernardino is here to guide you every step of the way. Our bilingual team helps you understand dental health options and insurance plans including Denti-Cal, PPO, and HMO to fit your budget and care needs.
Take charge of your dental care by visiting Monteluz Dental Specialty Group today where affordability and accessibility meet expert care. Contact us now for a personalized insurance review, clear cost estimates, and a treatment plan that works with your coverage. Don’t wait until a surprise bill delays important care. Learn all you need to know about your dental benefits at Dental Health Archives - Monteluz Specialty and schedule your visit to secure quality dental care with confidence.
Frequently Asked Questions
What is a deductible in dental insurance?
A deductible is the amount you must pay out of pocket for dental services before your insurance starts covering costs. Once you meet the deductible for the year, your insurance will begin to pay for covered procedures.
How does copay differ from coinsurance in dental plans?
A copay is a fixed amount you pay for specific services at the time of your visit, such as $25 for a filling. Coinsurance, on the other hand, is a percentage of the cost you pay after meeting your deductible, such as 20% of charges after the deductible is met.
What is the annual maximum in dental insurance?
The annual maximum is the cap on how much your insurance plan will pay for covered dental services in a calendar year. Once you reach this limit, you will be responsible for 100% of any further dental expenses until the next benefit year.
What are waiting periods in dental insurance?
Waiting periods are predefined times that you must wait before your dental insurance kicks in to cover certain procedures, like crowns or implants. These periods can vary by plan, so it’s important to understand them to avoid unexpected delays in necessary care.
Recommended
- Dental Insurance Explained: Making Care Affordable in California
- Affordable Dental Care Explained: Real Options in California
- 7 Essential Steps for a Family Dental Hygiene Checklist
- Dental Preventive Care: Protecting Families in California
