Why Dental Implants Fail – Key Risks for Families
Why Dental Implants Fail – Key Risks for Families

Worrying about the long-term success of dental implants is common for families who want reliable solutions at a fair price. With complications like peri-implantitis—an inflammatory disease that can damage bone and tissue—posing a real threat to implant stability, understanding the causes of implant failure becomes crucial for anyone investing in their smile. This guide will help you recognize risks, spot early warning signs, and choose the right specialty care in San Bernardino for safe, affordable dental restoration.
Table of Contents
- What Causes Dental Implants to Fail
- Different Types of Implant Failures
- Top Risk Factors for Implant Failure
- Recognizing Signs and Symptoms Early
- How to Prevent Dental Implant Failure
- What to Do if an Implant Fails
Key Takeaways
| Point | Details |
|---|---|
| Dental Implant Failure Factors | Key risk factors include poor oral hygiene, smoking, and chronic health conditions like diabetes. Managing these factors is crucial for implant success. |
| Types of Implant Failures | Implant failures can occur early, delayed, or late, each presenting unique challenges that require targeted approaches for management. |
| Monitoring Symptoms | Patients should be vigilant for signs of gum inflammation or implant instability, as early detection can prevent further complications. |
| Prevention Strategies | Effective prevention involves comprehensive pre-surgical evaluations, regular check-ups, and strong oral hygiene practices to maintain implant health. |
What Causes Dental Implants to Fail
Dental implant failure represents a complex challenge that can devastate patients hoping to restore their smile and dental function. Understanding the precise mechanisms behind implant complications helps families make informed decisions and protect their oral health investment.
Research indicates several critical factors contribute to dental implant failure. The University of Rochester Medical Center’s NIH-funded study highlights key biological disruptions that can compromise implant success:
- Peri-implantitis: An inflammatory disease damaging bone and surrounding tissue
- Chronic plaque accumulation around the implant site
- Inflammatory responses triggered by titanium particle release
- Compromised bone healing processes
- Systemic immune system challenges
Beyond biological factors, patients must also recognize lifestyle and medical conditions that significantly increase implant failure risks. The FDA’s comprehensive dental implant guidelines reveal several external contributors:
- Poor oral hygiene practices
- Persistent smoking habits
- Uncontrolled chronic diseases
- Compromised immune system functioning
- Active inflammatory conditions
Implant failure can manifest through various symptoms, including persistent pain, implant looseness, swelling, and unexpected mobility. These warning signs suggest potential underlying complications that require immediate professional evaluation.
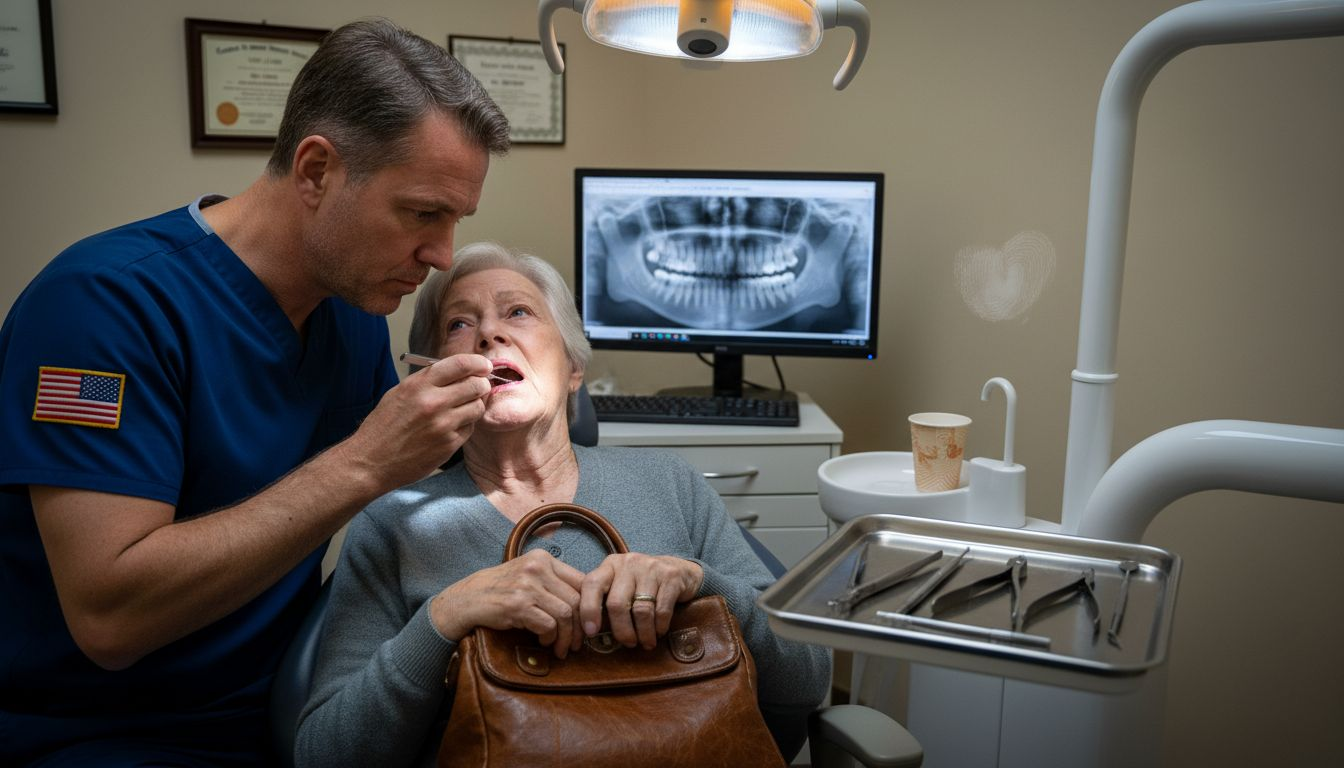
Patients with pre-existing conditions like diabetes, autoimmune disorders, or those undergoing specific medical treatments face heightened risks. Comprehensive health assessments and thorough pre-surgical screenings become crucial in determining individual implant candidacy.
Pro tip: Schedule a comprehensive oral health evaluation with your dental specialist to assess your specific implant success potential and develop a personalized prevention strategy.
Different Types of Implant Failures
Dental implant failures are not a uniform phenomenon but a complex spectrum of complications that can emerge at different stages of treatment and healing. Understanding the nuanced types of peri-implant diseases helps patients recognize potential warning signs and seek timely interventions.
Two primary categories of implant failures dominate clinical observations:
-
Peri-implant Mucositis: A reversible inflammatory condition
- Affects soft gum tissue surrounding the implant
- Characterized by redness and potential swelling
- No significant bone loss at this stage
-
Peri-implantitis: A more severe inflammatory condition
- Involves inflammation and progressive bone deterioration
- Requires surgical intervention
- Can lead to implant instability and potential removal
Implant failures can be further categorized based on their temporal occurrence:
-
Early Failure: Occurs before or shortly after osseointegration
- Typically within the first three to six months
- Often related to surgical complications
- May result from poor initial implant placement
-
Delayed Failure: Develops after successful initial integration
- Occurs months or years following implant placement
- Frequently associated with ongoing biological complications
- Potentially triggered by systemic health changes
-
Late Failure: Happens after extended period of successful function
- Can be related to long-term mechanical stress
- Might involve gradual bone loss or implant structural compromise
- Often connected to patient’s overall health trajectory
Understanding these failure mechanisms requires comprehensive assessment of individual patient factors, including oral hygiene practices, systemic health conditions, and ongoing maintenance strategies. Each failure type presents unique challenges that demand specialized diagnostic and treatment approaches.
Here is an overview of implant failure types and their clinical implications:
| Failure Type | Timing | Key Impact | Recommended Action |
|---|---|---|---|
| Early Failure | Before 6 months | Poor initial healing | Surgical reassessment |
| Delayed Failure | Months to years | Bone/tissue compromise | Investigate systemic causes |
| Late Failure | After years | Mechanical stress damage | Evaluate lifestyle/health |
Pro tip: Maintain regular dental check-ups and document any unusual symptoms around your dental implants to enable early detection of potential complications.
Top Risk Factors for Implant Failure
Dental implant success depends on a complex interplay of patient health, lifestyle, and biological factors. Research from the University of Rochester Medical Center reveals critical risk factors that can significantly compromise implant longevity and performance.
Physiological and medical risk factors play a crucial role in implant failure potential:
-
Chronic Health Conditions
- Diabetes
- Autoimmune disorders
- Compromised immune system
- Inflammatory diseases
- Hormonal imbalances
-
Lifestyle-Related Risks
- Persistent smoking
- Poor oral hygiene
- Excessive alcohol consumption
- High-stress environments
- Inadequate nutrition
Biological mechanisms that contribute to implant failure include:
-
Inflammatory Response Triggers
- Chronic inflammation around implant site
- Disrupted bone healing processes
- Compromised tissue integration
- Immune system overreaction
-
Mechanical and Structural Challenges
- Insufficient bone density
- Improper surgical placement
- Titanium particle release
- Micromovement of implant
- Occlusal stress
Patients with multiple risk factors face exponentially higher chances of implant complications. For instance, a smoker with diabetes and poor oral hygiene represents an extreme risk profile that dramatically reduces implant survival probability.
Precise diagnostic screening and comprehensive health assessments become critical in identifying potential barriers to successful implant integration. Understanding individual risk factors allows dental professionals to develop personalized treatment strategies that mitigate potential failure mechanisms.
Compare common risk categories contributing to dental implant failure:
| Risk Category | Examples | Effect on Implant Success | Prevention Strategies |
|---|---|---|---|
| Health Conditions | Diabetes, autoimmune disorders | Increased infection risk | Medical management, screenings |
| Lifestyle Factors | Smoking, poor hygiene | Higher inflammation/complications | Cessation, hygiene improvements |
| Biological Factors | Bone density, immune response | Reduced osseointegration | Pre-surgical assessment |
Pro tip: Conduct a thorough medical history review and lifestyle assessment with your dental specialist to proactively identify and address potential implant failure risks.
Recognizing Signs and Symptoms Early
Detecting potential dental implant complications requires vigilant monitoring and understanding of subtle warning signs in peri-implant diseases. Early recognition can prevent irreversible damage and preserve the long-term success of dental implant treatments.
Critical early warning signs that demand immediate attention include:
-
Gum-Related Symptoms
- Persistent redness around implant site
- Unexplained swelling or tenderness
- Bleeding during brushing or flossing
- Receding gum tissue near implant
- Unusual gum texture or appearance
-
Implant Stability Indicators
- Sudden or gradual implant movement
- Changes in bite alignment
- Discomfort while chewing
- Unusual clicking or shifting sensations
- Persistent pain or sensitivity
Patients should monitor these potential complications systematically:
-
Physical Sensation Assessment
- Track pain levels and character
- Note any changes in implant comfort
- Observe chewing and speaking patterns
-
Visual Inspection Protocols
- Check gum color and texture weekly
- Look for inflammation or discoloration
- Examine implant for visible changes
The Food and Drug Administration recommends immediate professional consultation if patients experience persistent inflammation, unusual pain, or implant mobility. Timely intervention can prevent advanced complications and potential implant loss.

Understanding that each patient’s healing process is unique helps manage expectations and promote proactive health monitoring. Some discomfort is normal during initial healing, but ongoing or worsening symptoms require professional evaluation.
Pro tip: Create a weekly self-examination routine to track your dental implant’s healing progress and document any changes to discuss with your dental specialist.
How to Prevent Dental Implant Failure
Preventing dental implant failure requires a strategic, comprehensive approach that encompasses multiple aspects of oral and overall health. Prevention strategies from periodontal experts emphasize proactive management and consistent care.
Critical prevention strategies include:
-
Pre-Surgical Preparation
- Comprehensive medical evaluation
- Detailed dental health screening
- Management of chronic conditions
- Blood sugar control for diabetic patients
- Nutritional optimization
-
Lifestyle Modification Factors
- Complete smoking cessation
- Stress reduction techniques
- Balanced nutrition
- Regular exercise
- Alcohol moderation
Effective oral hygiene protocols demand systematic attention:
-
Daily Maintenance Routine
- Specialized implant cleaning tools
- Soft-bristled toothbrush techniques
- Antimicrobial mouthwash
- Gentle flossing around implant sites
- Professional-grade interdental brushes
-
Professional Care Protocols
- Quarterly dental check-ups
- Professional cleaning
- Periodic implant stability assessment
- Radiographic evaluations
- Comprehensive oral health monitoring
Patients must recognize that implant success depends on a holistic approach combining meticulous personal care, professional oversight, and lifestyle management. Individual health profiles significantly influence long-term implant performance.
Maintaining open communication with dental professionals and adhering to personalized care instructions can dramatically reduce implant failure risks. Early intervention and proactive monitoring remain the most effective prevention strategies.
Pro tip: Develop a detailed dental implant care journal to track healing progress, document any changes, and maintain consistent communication with your dental specialist.
What to Do if an Implant Fails
Dental implant failure can be a distressing experience, but understanding the strategic management approaches recommended by medical experts provides a clear path forward. Prompt and informed action can mitigate long-term complications and potentially preserve future implant opportunities.
Immediate steps following implant failure include:
-
Initial Professional Consultation
- Schedule urgent dental appointment
- Bring detailed medical history
- Describe specific symptoms
- Request comprehensive evaluation
- Prepare for potential diagnostic imaging
-
Diagnostic Assessment Protocols
- Comprehensive oral examination
- Radiographic imaging
- Infection screening
- Bone density evaluation
- Systemic health review
Treatment pathways typically follow these critical stages:
-
Implant Removal Process
- Surgical extraction of failed implant
- Thorough site cleaning
- Infection management
- Potential bone grafting
-
Healing and Rehabilitation
- Prescribed antibiotics
- Wound care instructions
- Periodic monitoring
- Nutritional support
- Recovery planning
Patients must understand that implant failure does not definitively preclude future dental restoration. Many successful reimplantation scenarios emerge after comprehensive diagnostic work and targeted interventions.
The complexity of implant failure demands a personalized, multidisciplinary approach that considers individual health profiles, underlying conditions, and potential reconstructive strategies.
Pro tip: Maintain a detailed medical documentation trail to help your dental specialist develop the most effective recovery and reimplantation strategy.
Protect Your Family’s Smile with Expert Dental Implant Care
Understanding why dental implants fail is crucial for families who want lasting, reliable solutions to restore smiles and confidence. Challenges like peri-implantitis, immune system complications, and lifestyle risk factors such as smoking or uncontrolled diabetes can threaten implant success. These pain points highlight the importance of thorough evaluations and personalized prevention strategies to safeguard your oral health investment.
Take control of your dental health today by partnering with Monteluz Dental Specialty Group. Our bilingual specialists provide comprehensive assessments and advanced dental implant services tailored to your unique needs. With accessible care in San Bernardino and flexible payment options, we remove barriers so you can feel secure about your family’s smiles. Learn more about maintaining implant health through our Dental Health and start your journey at Monteluz Dental Specialty Group. Don’t wait until complications arise. Schedule your consultation now and invest in prevention and peace of mind.
Frequently Asked Questions
What are the main causes of dental implant failure?
Dental implant failure can be caused by several factors, including peri-implantitis, chronic plaque accumulation, inflammatory responses from titanium particle release, compromised bone healing, poor oral hygiene, smoking, uncontrolled chronic diseases, and an impaired immune system.
How can I identify early signs of dental implant failure?
Early signs of dental implant failure include persistent redness or swelling around the implant site, bleeding during brushing, gum recession, unusual implant mobility, discomfort while chewing, and persistent pain or sensitivity.
What lifestyle factors increase the risk of dental implant failure?
Lifestyle factors that increase the risk of dental implant failure include smoking, poor oral hygiene practices, excessive alcohol consumption, high-stress environments, and inadequate nutrition.
What should I do if my dental implant fails?
If a dental implant fails, it’s crucial to consult your dentist immediately for a comprehensive evaluation. They may recommend implant removal, infection management, and a tailored rehabilitation plan, which could include bone grafting for future implant placement.
Recommended
- 6 Key Types of Dental Implants for Affordable Family Care
- Dental Implants Missing Teeth Tooth Replacement
- Dental Implant Procedure: Transforming Smiles in San Bernardino
- Dental Implants: Transforming Oral Health in San Bernardino
